Side Effects And Risks Of Blood Thinners
Are you considering taking blood thinners to manage a health condition? Before deciding, you must know the potential side effects and risks involved.
Blood thinners, such as anticoagulant medications, are often prescribed to prevent blood clots and lower the chances of stroke or heart attack. However, knowing their potential side effects, including fatigue, is essential. Therefore, one might wonder, Does blood thinner make you tired? It’s essential to discuss any concerns with a healthcare professional for a better understanding of individual experiences and possible strategies to manage fatigue while taking blood thinners.
Side Effects of Blood Thinners
If you’re taking blood thinners, you should be aware of a few side effects and risks.
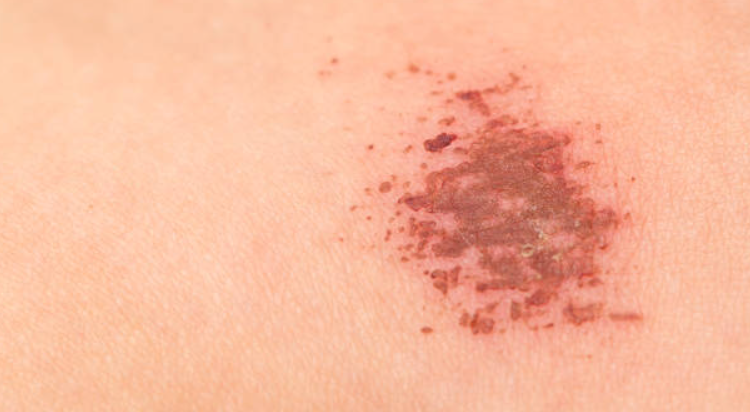
One common side effect is minor bleeding, such as nosebleeds or easy bruising. However, there is also a risk of severe bleeding, which can be life-threatening and require immediate medical attention.
Another potential side effect is nausea, which is usually temporary and can be managed with medication.
Additionally, blood thinners can increase the risk of spinal bleeding, leading to paralysis.
It is essential also to note that while blood thinners are used to prevent blood clots, there is a small risk of developing blood clots due to taking them.
Minor bleeding
Experiencing minor bleeding while taking blood thinners? Don’t worry; it’s a common side effect that can be easily managed.
Blood thinners, also known as anticoagulants, are prescribed to prevent blood clots from forming or treat existing clots. While they’re highly effective in reducing the risk of severe conditions like strokes and heart attacks, they come with some side effects and risks.
One of the most common side effects of blood thinners, including different types of blood thinners, is minor bleeding. Minor bleeding can occur in various forms, such as nosebleeds, bruising, or minor cuts that take longer to stop bleeding. Since blood thinners reduce the clotting ability of your blood, even a minor injury can result in prolonged bleeding. However, it’s important to remember that this usually isn’t a cause for concern.
Most cases of minor bleeding can be easily managed by applying pressure to the affected area or using over-the-counter products like adhesive bandages or nasal sprays. It’s also crucial to inform your healthcare provider about minor bleeding so they can monitor your condition and adjust your medication if necessary.
While minor bleeding is a common side effect of blood thinners, it’s essential to be aware of the potential risks associated with this medication. Since blood thinners prevent blood clots, they can also increase the risk of excessive bleeding in certain situations. Avoiding injuries or accidents that could lead to significant bleeding, such as wearing protective gear during physical activities or being cautious when using sharp objects, is crucial.
Additionally, it’s essential to communicate with your healthcare provider about any changes in your health or medications, as they can provide guidance on managing the risks and benefits of blood thinners.
Experiencing minor bleeding while taking blood thinners is a common side effect that can be easily managed. By taking appropriate precautions and promptly addressing any instances of bleeding, you can minimize the impact of this side effect. Remember to discuss any concerns or changes in your condition with your healthcare provider to ensure the risks and benefits of blood thinners are appropriately monitored and balanced.
Serious bleeding
Don’t ignore any signs of severe bleeding while on blood thinners; seek immediate medical attention to ensure your safety. Serious bleeding is a potential side effect of blood thinners and should never be taken lightly.
If you notice any unusual bleeding that doesn’t stop or experience excessive bruising or blood in your urine or stool, it is essential to act quickly. Contact your healthcare provider or go to the nearest emergency room right away. They’ll be able to assess the situation and provide you with the necessary medical intervention to stop the bleeding and prevent any further complications.
Severe bleeding can occur in different parts of the body and can range from mild to severe. It may present as prolonged nosebleeds, heavy menstrual bleeding, or bleeding gums. In more severe cases, it can manifest as blood in the brain, which can lead to a stroke, or blood in the stomach or intestines, which can cause internal bleeding. These situations require immediate medical attention to prevent any life-threatening consequences.
Remember, the key is not to promptly ignore signs of severe bleeding and to seek medical help. Your healthcare provider can guide you on the appropriate steps to take and ensure your safety while on blood thinners.
Nausea
When taking blood thinners, you must know that you may experience nausea as a potential side effect. Nausea is a common symptom that can occur when your body is adjusting to the medication.
It may feel like an unsettled stomach, queasiness, or the urge to vomit. While it can be uncomfortable, it is usually temporary and goes away as your body gets used to the blood thinner.
If you find that the nausea persists or becomes severe, it’s essential to contact your healthcare provider for further guidance.
To help manage nausea while taking blood thinners, taking your medication with food or a light snack is recommended. This can help to minimize stomach irritation and reduce the likelihood of nausea. Also, avoid spicy or greasy foods that may worsen your symptoms.
If you experience nausea, taking slow, deep breaths and finding a comfortable, relaxing position may also be helpful. If nausea persists or becomes severe, or if you notice any other concerning symptoms, it’s essential to seek medical attention as soon as possible.
Spinal bleeding
Be aware of the potential for spinal bleeding while on blood thinners – it’s crucial to understand the risks involved. Blood thinners are medications that help prevent blood clots but can also increase the risk of bleeding.

Spinal bleeding, also known as spinal hematoma, occurs when there is bleeding in or around the spinal cord. This can be a severe condition that may lead to paralysis or other neurological complications.
When you’re on blood thinners, the risk of spinal bleeding increases if you have an injury or undergo a spinal procedure, such as a spinal tap or spinal anesthesia, it’s essential to inform your healthcare provider that you’re taking blood thinners before any spinal procedure, as they may need to adjust your medication or take other precautions to minimize the risk.
Symptoms of spinal bleeding may include severe back pain, weakness or numbness in the legs, difficulty walking or moving, and loss of bowel or bladder control. If you experience any of these symptoms, seeking immediate medical attention is crucial. Prompt diagnosis and treatment of spinal bleeding can help prevent further damage and improve outcomes.
While blood thinners can be lifesaving medications, it’s essential to be aware of the potential risks, including spinal bleeding. Understanding these risks and taking necessary precautions can help ensure your safety while on blood thinners. Remember to communicate with your healthcare provider and seek immediate medical attention if you experience any concerning symptoms.
Blood clots
To fully understand the potential dangers of spinal bleeding, you must know the risks associated with blood clots. Blood clots are a common side effect of blood thinners, medications designed to prevent blood from clotting too quickly.
While blood thinners can effectively reduce the risk of stroke and other cardiovascular events, they can also increase the risk of developing blood clots in certain situations. This is because blood thinners slow the body’s natural clotting process, sometimes leading to an imbalance between clotting and bleeding.
When blood clots form within blood vessels, they can obstruct blood flow and cause serious complications. If a blood clot forms in a deep vein, it can lead to a condition known as deep vein thrombosis (DVT), which most commonly occurs in the legs. If a DVT is not treated promptly, the clot can break free and travel through the bloodstream to the lungs, causing a potentially life-threatening condition called a pulmonary embolism.
Blood thinners can increase the risk of developing blood clots in individuals who have certain medical conditions or who have undergone certain surgeries, such as joint replacement surgery. It’s essential to work closely with your healthcare provider to monitor your risk of blood clots while taking blood thinners and to promptly report any signs or symptoms of a potential clot, such as swelling, pain, or redness in your legs.
Risks of Blood Thinners
Too much blood thinner can lead to an overdose, which can be dangerous.
One of the risks of blood thinners is the increased chance of experiencing a hemorrhagic stroke, which occurs when a blood vessel in the brain bursts.
Internal bleeding is another potential risk, as blood thinners can make it difficult for your blood to clot properly.
Additionally, blood thinners can interact with other medications you may be taking, so it’s essential to be aware of potential drug interactions.
Overdose of Blood Thinner
When taking blood thinners, being aware of an overdose’s potential risks and side effects is crucial, as this can lead to severe complications and put your health at risk.
An overdose of blood thinners can cause excessive bleeding, which can be life-threatening. You may experience prolonged or uncontrollable bleeding from cuts, bruises, or minor injuries. Additionally, you may notice blood in your urine, stools, or vomit, which are signs of internal bleeding.
It’s essential to seek immediate medical attention if you suspect an overdose, as prompt treatment can be critical in preventing further complications.
In addition to excessive bleeding, an overdose of blood thinners can also increase the risk of developing blood clots. Paradoxically, while blood thinners are prescribed to prevent blood clots, too much can disrupt the delicate balance and promote clot formation. This can lead to conditions like deep vein thrombosis (DVT) or pulmonary embolism, which can be life-threatening.
If you experience sudden pain, swelling, redness in your legs, or difficulty breathing, you must seek medical help immediately.
Taking the prescribed dosage of blood thinners and closely monitoring your INR levels can help prevent an overdose and minimize the risks associated with these medications.
Hemorrhagic Stroke
Excessive blood thinners can lead to a potentially life-threatening complication known as a hemorrhagic stroke. This occurs when there is bleeding in the brain, which can cause severe damage and even death. The risk of a hemorrhagic stroke increases when blood thinners are taken in higher doses than prescribed or combined with other medications that also thin the blood.
It is essential to follow your doctor’s instructions carefully and never exceed the recommended dosage of blood thinners to avoid this dangerous side effect. Suppose you experience symptoms such as sudden severe headache, weakness or numbness on one side of the body, difficulty speaking, or loss of coordination. In that case, it is crucial to seek immediate medical attention. These may be signs of a hemorrhagic stroke, and prompt treatment is essential to minimize the potential damage.
In some cases, emergency surgery may be required to stop the bleeding and relieve the pressure on the brain. Remember, taking too much blood thinner can have serious consequences, so always consult your healthcare provider and never change your medication regimen without their guidance. Your health and well-being should always be the top priority.
Internal Bleeding
Internal bleeding can be a severe complication that needs immediate medical attention. If you’re taking blood thinners, you may be at a higher risk of experiencing internal bleeding. Blood thinners reduce the blood’s ability to clot, which can be beneficial in preventing blood clots. However, it also means that any injury or trauma to the body can result in prolonged bleeding.
Internal bleeding can occur in various body parts, such as the brain, stomach, or intestines, including during pregnancy. When it comes to pregnant women, using blood thinners in pregnancy requires careful consideration. Suppose you experience severe pain, dizziness, or weakness or notice blood in urine or stool. In that case, it’s crucial to seek immediate medical help to address any potential complications related to blood thinners in pregnancy.
It’s vital to act quickly to stop the bleeding and address the underlying cause when internal bleeding occurs. Your healthcare provider may recommend interventions such as blood transfusions, surgery, or medication to manage the bleeding. It’s essential to follow their instructions closely and inform them about any changes in your symptoms.
Remember, if you’re on blood thinners, balancing preventing blood clots and minimizing the risk of internal bleeding is crucial. Be proactive in discussing any concerns or questions with your healthcare provider, as they can guide you in managing your condition effectively and reducing the risk of complications.
Difficulty Stopping Bleeding
Acting quickly and addressing difficulty stopping bleeding to prevent further complications is crucial. If you’re experiencing difficulty stopping bleeding while taking blood thinners, seeking immediate medical attention is essential.
Blood thinners reduce the blood’s ability to clot, which prevents harmful blood clots. However, this also means that even minor cuts or injuries can lead to excessive bleeding.
If you notice that bleeding from a cut or wound is not stopping or is taking longer than usual to clot, it’s essential to inform your healthcare provider as soon as possible. They can assess the severity of the situation and provide appropriate guidance or treatment to help control the bleeding.
Sometimes, healthcare professionals may need to adjust your blood thinner dosage or temporarily stop the medication to allow the bleeding to stop. They may also recommend applying direct pressure to the bleeding site, elevating the affected area, or using ice packs to constrict blood vessels and reduce bleeding.
It’s crucial not to ignore difficulty stopping bleeding, as it can lead to excessive blood loss, which may be life-threatening in severe cases. By promptly addressing this issue with your healthcare provider, you can ensure proper management and minimize the risks associated with blood thinners.
Remember, never make any changes to your medication without consulting your doctor first, as they’re best equipped to provide personalized advice based on your situation.
Drug Interactions
If you thought difficulty stopping bleeding was the only concern when taking blood thinners, think again. Another essential factor to consider is the potential for drug interactions.
When you take blood thinners, you must know how they can interact with other medications you may be taking. These interactions can sometimes lead to serious side effects or reduce the effectiveness of the blood thinner, putting your health at risk.
Certain medications can increase the risk of bleeding when combined with blood thinners. For example, nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or aspirin can interfere with the blood’s ability to clot, compounding the effects of blood thinners. Some antibiotics, antifungal medications, and anticoagulants can also interact with blood thinners, amplifying their effects or causing adverse reactions.
To ensure the safe and effective use of blood thinners, it is crucial to inform your healthcare provider about all your medications, including over-the-counter drugs, herbal supplements, and vitamins. Your doctor can assess the potential interactions and adjust your treatment plan accordingly, minimizing the risks and maximizing the benefits of blood thinners in your case.
Conclusion
In conclusion, blood thinners can be an effective treatment for various medical conditions, but they’re not without their risks and side effects. Before starting this medication, weighing the potential benefits against the potential drawbacks is essential.
While blood thinners can help prevent blood clots and reduce the risk of stroke or heart attack, they can also increase the risk of bleeding and bruising. It’s crucial to carefully monitor your health and promptly report any unusual symptoms or side effects to your healthcare provider.



