How did Blood Thinners work to Prevent Clots?
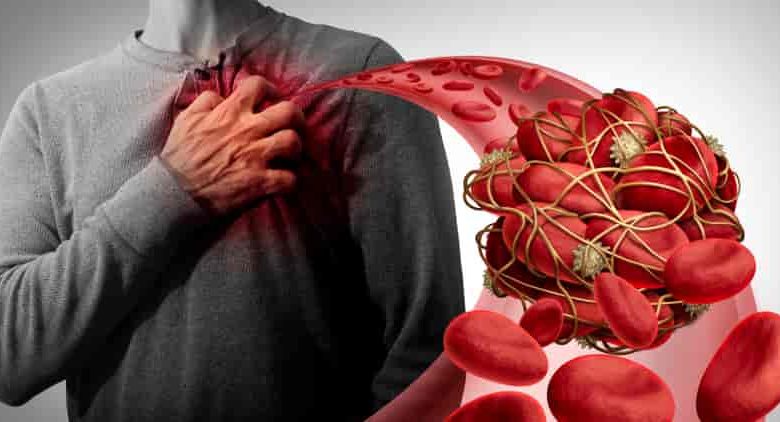
Clots that form in the arteries, veins, and heart can lead to heart attacks, strokes, and blockages that can cause other health problems. Blood thinners minimize the process of blood clotting. Currently, there are numerous blood thinners on the market. Anticoagulants like warfarin and Xarelto work by slowing down the body’s process of clot formation, while antiplatelets, like Eliquis, prevent the blood cells from sticking together.
They are either anticoagulants or antiplatelets. You must consult your doctor before consuming either of them. Because A common concern among users is potential side effects, such as Does Xarelto make you tired? And other similar queries. Depending on your condition and health history, you have been prescribed thinners like Warfarin, Xarelto, and Eliquis. To determine the right kind, you must understand the mechanism of how blood thinners work to prevent clots.
Mechanism Of Blood Thinners
Blood thinners’ main aim is preventing blood clotting. 2 to 3 million patients consume these thinners annually. These drugs do not affect the existing clots but do not let new clots form either.

After the consumption of thinners, it goes through multiple processes like absorption, circulation, and targeting the affected area before beginning to work on it. If your thinner is an anticoagulant, it hampers the process of clot formation, essentially reducing the clot formation.
If your thinner is an antiplatelet agent, it interferes with platelet activation and aggregation. Stopping the platelet formation process reduces the chances of platelets sticking together to form a clot.
There are different medications to eliminate existing clots, but thinners aren’t the ones. Several new patients have such inhibitions, so here is a detailed description of how blood thinners work to prevent clots.
Inhibition of Clotting Factors
- The majority of thinners hamper clotting factors in the blood. Heparin and fondaparinux, for instance, work well with antithrombin III. Together they deactivate clotting factors such as factor Xa and thrombin.
- Similarly, Warfarin hampers the liver’s production of vitamin K-dependent clotting factors (II, VII, IX, X).
- Clotting factors such as factor Xa and thrombin are directly inhibited by DOACs (Direct Oral Anticoagulants).
Interference with Platelet Activation
- Antiplatelets deactivate platelet aggression and activation.
- Medications like aspirin, clopidogrel, and ticagrelor, hamper the platelet activation and aggregation process.
- Platelets play a vital role in the clot formation process as they clump together at the injury site.
- Antiplatelets hinder the production of platelets to a great extent.
Promotion of Anticoagulant Proteins
- Some synthetic anticoagulants increase the effectiveness of natural anticoagulant proteins. Such thinners fasten the process of healing.
- Drugs like Heparin enhance the effectiveness of antithrombin III, which hinders clotting factors.
- Direct thrombin inhibitors, such as argatroban and bivalirudin, directly bind and affect thrombin activity, an essential clotting factor.
Disruption of Clotting Cascade
- During the inhibition process, certain thinners target specific steps.
- These thinners interfere with the procedures of specific clots-forming agents and enzymes.
- This hinders the clot formation process by delaying the process.
Using Blood Thinners: Dos and Don’ts
Blood thinners are usually consumed by patients who suffer from severe issues like deep vein thrombosis (DVT), which leads to pulmonary embolism. It is known that nearly 900,000 American citizens suffer from DVT. Women, especially in their later ages, suffer from the disease because of high-stress levels and frequent consumption of birth control pills. This happens because the blood begins to clot.
Serious illnesses, injuries, obesity, and long periods of inactivity can also increase your risk of blood clotting. You must consult your healthcare provider if you are at a high risk of infesting the disease. If they recommend you begin with blood thinners, such as Warfarin or other medications, you should immediately work on the advice. Understanding the effects of various blood thinners is crucial in managing your condition and reducing the risk of complications.
However, you must gain as much information as possible before consuming it. While understanding how blood thinners work, you must also learn the dos and don’ts. Here’s a list of a few shoulds and shouldn’t you can begin with:
Shoulds:
- Keep an eye on any new bruises or increased bleeding.
- Get your blood checked now and then. Being in tandem with your health can help your healthcare provider reduce or increase your dosage.
- You must inform your healthcare provider beforehand if you have any other health condition.
- You must consult your doctor before stopping any medications.
- Wearing a medical bracelet can help you a lot.
- If traveling is necessary, you must plan and keep yourself hydrated.
- Stay active as much as possible.
- You must avoid mixing vitamins with your medications, especially when considering the role of blood thinners in heart disease. Some vitamins might not sit well with your medication, causing you to bleed or hamper the effectiveness of the thinner.

Shouldn’ts
- Never stop eating green vegetables.
- Do not sit for prolonged hours if you’re traveling.
- If you bruise majorly, you must not delay seeing a doctor.
- When shaving regularly, you do not need to worry about getting nicked. It wouldn’t cause you great harm.
- Alcohol is an absolute no-no.
- You don’t need to stop your blood thinning medication before any other appointment.
- If you miss out on any of your doses, you must not take a double dose the next time.
The Bottom Line
It is essential to learn how blood thinners work to prevent clots before consuming any sort of blood-thinning drug. Every thinner works in its own way; however, the main idea of the mechanism of action can either be anticoagulation or antiplatelet activation.
One must also be acquainted with the kind of thinner they are to consume and what they should and should not do while they continue with their procedure.
How long does it take a blood clot to dissolve with blood thinners?
Depending on the size of the clot, a blood thinner would dissolve it within a few weeks, or it may take months to dissolve. However, once the clot has dissolved, the chances of it reappearing or forming again are quite less.
What blood thinner breaks up clots?
Anticoagulants, such as heparin, warfarin, dabigatran, apixaban, and rivaroxaban, are medications that thin the blood and help to dissolve blood clots.
Can you live a long life on blood thinners?
It might alter your lifestyle, but it is possible to lead a healthy and active lifestyle. Leading an active lifestyle can, in turn, help you in reducing the risk of blood clotting, ultimately benefitting you with a long life.